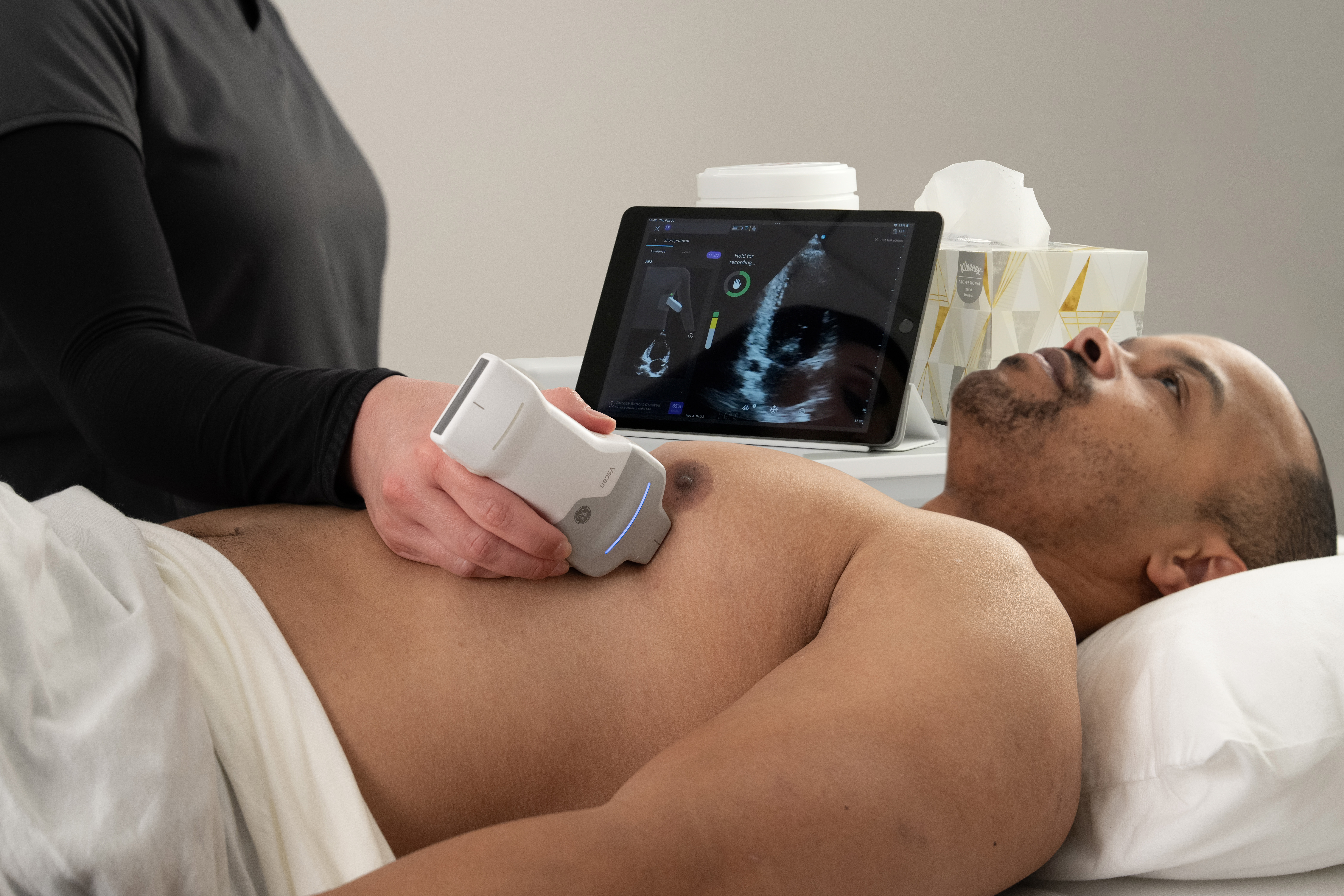
Echocardiography is a prime example of how artificial intelligence (AI) is reshaping healthcare. Earlier this year GE HealthCare announced the availability of Caption AITM & Caption GuidanceTM on its Vscan AirTM SL handheld ultrasound device, in addition to the VenueTM Point of Care Family. This AI integration provides bedside echo users with real-time, step-by-step scan guidance, including prompts on probe movements, to ensure they capture diagnostic-quality images. Caption AI also automatically calculates left ventricular ejection fraction (LVEF), a crucial measure in diagnosing and assessing various cardiac conditions, particularly heart failure.
The implications of AI assistance in rapid point-of-care cardiac assessments are profound. It empowers more clinicians of all experience levels to confidently capture diagnostic quality images so they can make timely, well-informed treatment decisions. The advantages of AI in focused echocardiography also reverberate within echo lab operations, where it creates potential for new levels of efficiency
Challenges facing the echo lab
Echo labs are under strain. Globally, the annual tally of echocardiography exams stands at 108 million1 and it is expected to remain a mainstay of patient care. This demand for resources is compounded by workforce challenges. The U.S. Bureau of Labor Statistics forecast an overall sonographer shortfall as experienced technologists are leaving the workforce for varying reasons. The demand for cardiac sonographers is particularly high due to the specialized nature of their work and the growing need for cardiovascular diagnostics3. The aging population significantly contributes to this demand, as older adults are more likely to require cardiovascular care.
For many echo labs these factors translate into a significant backlog of echocardiogram appointments, which in turn prolong patient wait time. Echo labs must find ways to optimize resource utilization and provide timely access to diagnostics for patients amid escalating echo exams volume.
The bedside echo connection
Providers across a range of clinical areas including primary care, internal medicine, emergency and critical care, women’s health, and pulmonary medicine are beginning to integrate handheld ultrasound devices into their standard toolkits. Evidence already shows that their use can lead to faster, safer, more accurate, and more affordable patient care3.
The widespread availability of handheld ultrasound devices represents a significant shift in cardiac care. Echocardiography is crucial for assessing cardiac structure and function, aiding in diagnosing and managing cardiovascular conditions. Traditionally conducted in specialized echo labs, point-of-care ultrasound now allows for focused bedside, ambulance, or home-based cardiac assessments, decentralizing access to these exams.
Though a potentially powerful diagnostic aid, the experience level of the clinician conducting a rapid cardiac assessment at the point of care impacts clinical next steps. Newer users may obtain images with limited visibility of cardiac structures or artifacts. There is also the potential for false positives which can unnecessarily consume cardiology resources. The prevalence of unneeded echo lab referrals is already a general utilization concern being looked at globally—a recent study found that, among patients without known cardiovascular disease who were referred for an echo due to chest pain, dyspnea, or palpitations, between 62-87% of cases did not have abnormal cardiac findings4.
AI at the bedside has a ripple effect
Adoption of AI-driven scan guidance could significantly reduce the learning curve for ultrasound usage, and as a result, optimize the cardiac care pathway. This can trigger a number of operational benefits in the echo lab.
-
Facilitate early triage and prioritization: Enable prompt identification of relevant findings, allowing clinicians to prioritize cases requiring immediate attention and allocate resources efficiently.
-
Mitigate unnecessary exams and transfers: Curb unneeded referrals to the echo lab and reduce the need for patient transfers.
-
Optimize resource utilization: Ensure efficient use of resources by enabling the echo lab to focus on critical cases, and potentially reduce the need for urgent specialist consultations
-
Minimize backlog and reduce wait times: Improve backlog clearance rate, leading to reduced wait times for non-urgent echocardiograms.
Above all, the adoption of AI guidance in focused cardiac assessments has exciting potential for improving patient experience. Patients can benefit from prompt initiation of appropriate interventions or reassurance if no significant abnormalities are detected.
REFERENCES
- Poornima Srinivasan, “Healthcare Infrastructure and Procedural Volume for Ultrasound Imaging,” Frost & Sullivan, 2018. Calculation based on 26% total global prevalence of CVD cases (422 million) undergoing echo exam; extrapolated from US study indicating roughly 26% of total prevalent CVD cases underwent echo exams percentage value validated from reports. https://www.gehealthcare.com/-/jssmedia/gehc/us/files/products/ultrasound/vivid/redesign/updated-brochures/brochure_echolab-vivid-ultra-edition_jb20772xx-updated.pdf?rev=-1 )
- “Growing Demand for Cardiovascular Sonographers,” Ultrasound Technician Center, last modified 2024, https://www.ultrasoundtechniciancenter.org/specialized-programs/demand-for-cardiovascular-sonographers.html. –or— Desiree Montilla, “VCU Health addressing cardiac sonographer shortage,” Richmond 12, last modified February 23, 2024, https://www.12onyourside.com/2024/02/23/vcu-health-addressing-cardiac-sonographer-shortage/.
- Adam Hsieh et al., “Handheld Point-of-Care Ultrasound: Safety Considerations for Creating Guidelines,” Journal of Intensive Care Medicine 37, no. 9 (2022): 1146-115.
- Sher May Ng et al., “Feasibility, diagnostic performance and clinical value of an abbreviated echocardiography protocol in an out-patient cardiovascular setting: a pilot study,” Echo Research and Practice 9, no. 8 (2022).
JB29599XX